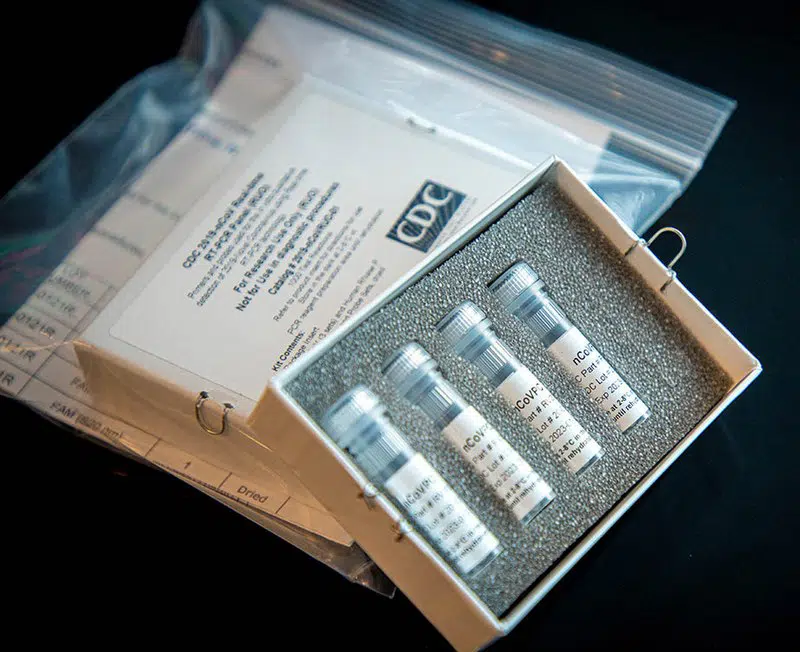
Home Covid-19 test kits will be covered by insurers starting Saturday, according to an announcement from the Biden Administration on Monday.
As of January 15, private health insurers will be required to cover up to eight home Covid-19 tests every month for their members. The news was welcomed as the country experiences a huge spike in the number of those testing positive for the Omicron variant of the virus and as they must test multiple times before they are allowed to take part in work or school after a diagnosis.
The Associated Press reports that as of Saturday, Americans will be able to either purchase home testing kits for free under their policies or ask for their insurance companies to reimburse them, according to whatever their monthly per-person limit would be.
A family of four may be able to be reimbursed for up to 32 tests every month — something that comes as a relief to families who are many times struggling just to get the tests in the first place.
As is already the case, PCR tests and rapid tests that have been ordered or administered by a health provider will continue to be fully covered by insurance with no limits whatsoever.
As the Omicron variant loomed on the horizon in December and as hospitals were grappling with record numbers of patients presenting with the Delta variant, President Biden faced mounting criticism as it became clear that there was a nationwide shortage of at-home tests.
Meanwhile the CDC and state health authorities were admonishing all those planning to visit relatives over the holiday season to take the test before their departure.
The Biden Administration faced withering criticism from those who compared the US’ comparable dearth of tests to the situation elsewhere, for example in Europe, where countries are sending free tests home to their citizens.
Later in January, the federal government will begin sending up to 500 million at-home test kits to Americans via a new website. In addition, the government and states are ramping up large-scale public testing sites in armories and other venues where there are the largest spikes in the virus.
This new development means that testing costs will soon be much less of a burden on American families at a time when they are trying to keep children in school while outbreaks of the virus continue in every county in every state in the country.
Health and Human Services Secretary Xavier Becerra said in a statement on Monday “This is all part of our overall strategy to ramp up access to easy-to-use, at-home tests at no cost. By requiring private health plans to cover people’s at-home tests, we are further expanding Americans’ ability to get tests for free when they need them.”
As part of its campaign to curb the spread of the virus and help ease the burden on families, the Biden administration has attempted to encourage private insurers to cover the tests up-front. doing away with the sometimes difficult reimbursement process.
Becerra stated that insurers who work together in tandem with pharmacies and retailers to cover the costs of the tests at point of sale will be required to reimburse only up to $12 per test if it is bought through an out-of-network retailer, however.
An incentive here is that those insurance companies that fail to act proactively to create a network of pharmacies they will work with will be faced with covering the full retail price of the tests, which could exceed $12 per test.
Responding to the news, the two largest health insurance industry groups in the US said that insurers would indeed work with the administration’s order, but cautioned that the process will not be all smooth sailing.
“Health insurance providers will work as quickly as possible to implement this guidance in ways that limit consumer confusion and challenges,” stated Matt Eyles, president of America’s Health Insurance Plans. “While there will likely be some hiccups in early days, we will work with the administration to swiftly address issues as they arise.”
Meanwhile, the Blue Cross Blue Shield Association directed concern toward the dearth of tests available for purchase. “We are concerned that the policy does not solve for the limited supply of tests in the country and could cause additional consumer friction as insurers stand up a program in just four days’ time,” stated Kim Keck, the group’s president, according to an Associated Press report.
There will be no retroactive clause in the new ruling so only those tests purchased beginning January 15 will be eligible for reimbursement; however, some insurers may elect to cover the costs of tests purchased earlier.
Having to shell out full price for the necessary tests to keep up with the ever-shifting recommendations and requirements of school, work and other activities has laid a further burden on families as they chase testing supplies in different pharmacies.
Mina Bressler, who is a mother of two in San Mateo, California, was able to locate some rapid test kits online; she was then generous enough to share some of them with another parent who also works outside the home, who she says doesn’t have time to “sit at her computer every hour refreshing the Walmart page to see when tests are in stock.
“I gave her some and her kids went to school. That’s one time and there’s a million of her,” Bressler explained.
“Just like vaccines becoming available really shone a light on the inequity of what’s going on in this pandemic, I think testing is the new flashlight for that because who’s going online stalking Walmart? It’s not the most vulnerable people in the county,” she went on to note.
Older Americans will not be able to have Medicare reimburse their tests; however, Medicaid and Children’s Health Insurance Program plans must cover the cost of at-home tests fully, according to the new ruling.
In addition, all those who are not on a covered insurance plan will be able to receive free tests through the new federal website — which should be online in the next couple of weeks — or from certain local community centers and pharmacies.
See all the latest news from Greece and the world at Greekreporter.com. Contact our newsroom to report an update or send your story, photos and videos. Follow GR on Google News and subscribe here to our daily email!



